3C Patch®: the evidence-based solution for diabetic foot ulcers
Diabetic foot ulcers are a common and severe complication of diabetes, and if left untreated, they can lead to chronic wounds, amputation, and even death.
Studies show that between 19 – 34% of persons with diabetes are likely to develop a foot ulcer.
Furthermore, only 30% of diabetic foot ulcers heal in 12 weeks, even with specialized outpatient wound care.

100% AUTOLOGOUS, EVIDENCE-BASED FOOT ULCER TREATMENT
Clinically proven to heal more wounds faster
3C Patch® addresses the unmet clinical need of diabetic foot ulcers that are not healing despite the best standard of care. Furthermore, 3C Patch® aims to reduce the number of diabetes foot ulcer patients who could otherwise potentially suffer from an amputation.
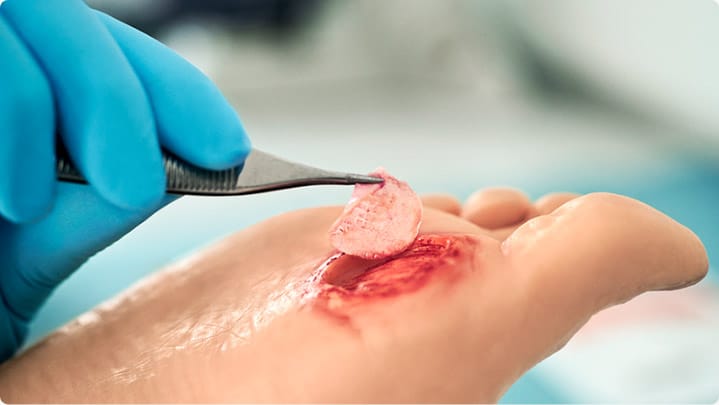
It takes approximately 20 minutes to prepare a 3C Patch® at the point of care. It is made entirely from the patient’s own blood and applied to the wound immediately thereafter. 3C Patch® is the 100% autologous, evidence-based foot ulcer treatment that is clinically proven to accelerate and support the body’s healing process.
ENTIRELY ALIVE
3C Patch® delivers key components found in the blood directly at the wound site
With just a small sample of the patient’s blood, the 3C Patch® System uses optical technology to automate the centrifugation process, which reformulates the blood into a triple-layer patch comprising fibrin, living cells, and growth factors that are released into the wound. Fibrin provides moisture retention; leukocytes are known to fight infection, while platelets are known to provide high growth factor levels and participate in the resolution of inflammation.
3C Patch® is an advanced wound care treatment that contains living cells, is 100% autologous, with no additives or reagents, and is created through a remarkably simple and automated process at the point of care.


REMARKABLY SIMPLE AND TIME-EFFICIENT
Produced on-demand from the patient’s own blood
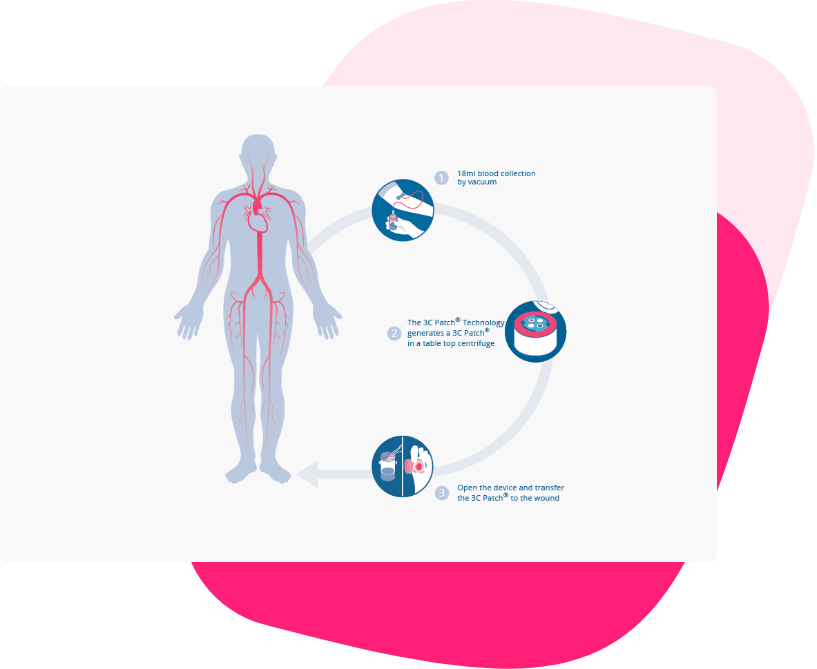
In a simple and time-efficient 20-minute process at the point of care, the 3C Patch® System produces a fully autologous biological wound treatment. It just requires an 18ml sample of the patient’s own blood, which is drawn directly into the 3C Patch® Device. The device is placed in the 3CP® Centrifuge, which in three steps automatically centrifugates, coagulates, and compacts components into a solid patch.
The 3C Patch® is then applied directly to the patient’s wound once a week.
How do diabetic foot ulcers form?
Due to a high blood sugar level, people with diabetes often develop nerve damage that prevents them from feeling pain in their limbs, either partially or entirely.
This neuropathy leads to loss of protective sensation radically increasing the risk of ulceration from accidental trauma or from ill-fitting footwear.
Furthermore, foot tissue can become ischemic because of macrovascular disease (atherosclerosis) but also as a result of neuropathy-based microvascular disease (e.g., vasomotor neuropathy and abnormal endothelial function). Protective sweating is lost, the skin of the ischemic foot is red and dry, with dystrophic nails, and susceptible to the pressure from a shoe or even an adjacent toe.
Bacterial infection, tissue ischemia, continuing trauma, and poor management can cause diabetic foot ulcers to heal slowly and transform readily into chronic wounds.
Approximately 60% of patients with diabetic foot ulcers develop wounds that become hard-to-heal.
DIABETES FOOT ULCERS (DFUs)
Key facts about diabetic foot ulcers1
DFUs represent an enormous public health issue causing ~250,000 annual hospitalizations and >$11B cost to US healthcare payors
Unhealed foot ulcers significantly decrease Quality of Life scores
The lifetime risk of a foot ulcer for any person with diabetes is around 25%
20% of DFU patients have major/ minor amputations within 1 year
The 4-year survival rate after major amputation is 35% and 55% after minor amputation
3C Patch® in a nutshell
Watch the video
Principles of foot ulcers treatment according to the International Working Group on Diabetic Foot
“Every 20 seconds somewhere in the world, someone loses a leg due to the complications of diabetes. At this moment, millions of people with diabetes suffer from poorly healing foot ulcers.”
The International Working Group on the Diabetic Foot is a multidisciplinary team of healthcare professionals in the field of diabetes and wound care that aims to create evidence-based guidelines for the prevention and management of diabetic foot disease.
Principles of ulcer treatment
Relief of pressure and protection of the ulcer
Restoration of skin perfusion
Treatment of infection
Metabolic control and treatment of comorbidity
Local wound care for treating foot ulcers
Debride the ulcer (with a scalpel), and repeat as needed
Select dressings to control excess exudation and maintain a moist environment
IWGDF Guidelines 2019 describe 3C Patch® as an autologous combined leukocyte, platelet, and fibrin construct and recommend it as an adjunctive treatment for diabetic foot ulcers that are difficult to heal.
Results obtained with 3C Patch® on different types of foot ulcers
Clinical studies
A multicenter cohort study evaluated the clinical performance of 3C Patch® in chronic DFU’s intending to assess the effect of treatment on area reduction and healing rate (complete wound closure at 12 and 20 weeks). 3C Patch® was applied once a week for up to 19 treatments or until the target ulcer was completely epithelized. More than 70% of ulcers with a duration between 8-25 weeks healed.
An independent, observer-blinded, and multicenter RCT involving 32 international centers and 269 hard-to-heal DFU patients evaluated the effectiveness of 3C Patch® on hard to heal diabetic foot ulcers.
It was published in The Lancet, September 2018, and demonstrates that 3C Patch® significantly increases the chance of wound closure compared to the best standard of care.
Patient case reports
In addition to the clinical studies results, 3C Patch® has also proven effective in clinical practice on diabetic foot ulcers that failed to heal for weeks or even years.
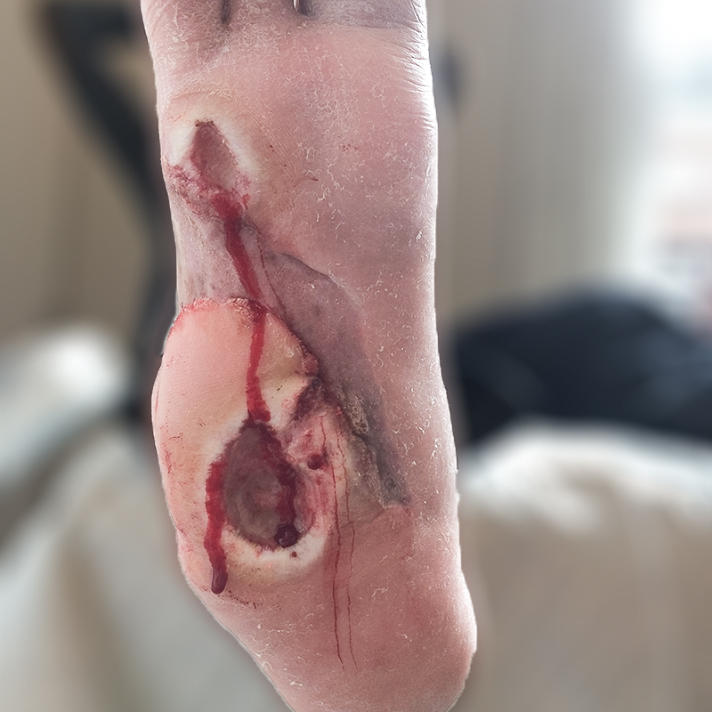
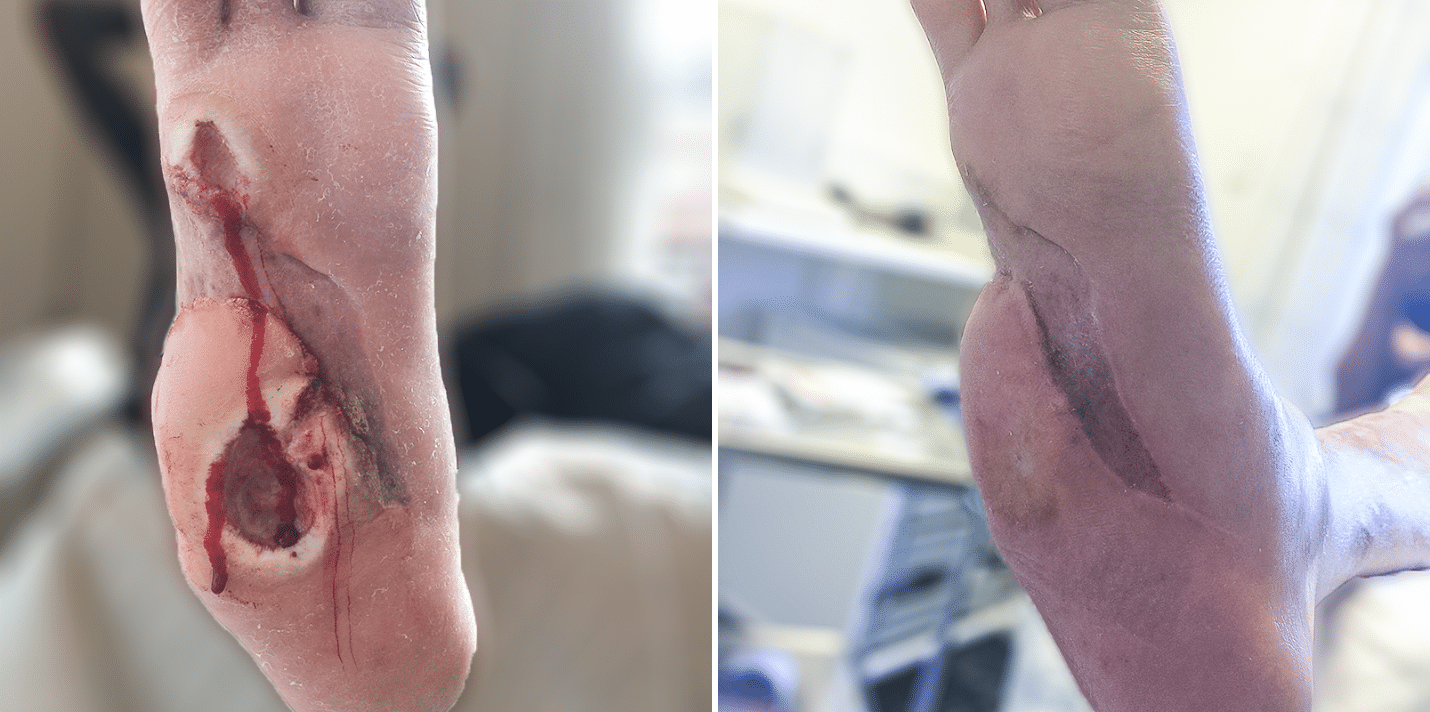
Diabetic foot ulcer
36-year-old, Male, Type 1 Diabetes diagnosed age 12, Informed by local hospital that amputation was the next step because the foot ulcer had not healed after 2.5 years of treatment
One 3C Patch® application per week for 11 weeks
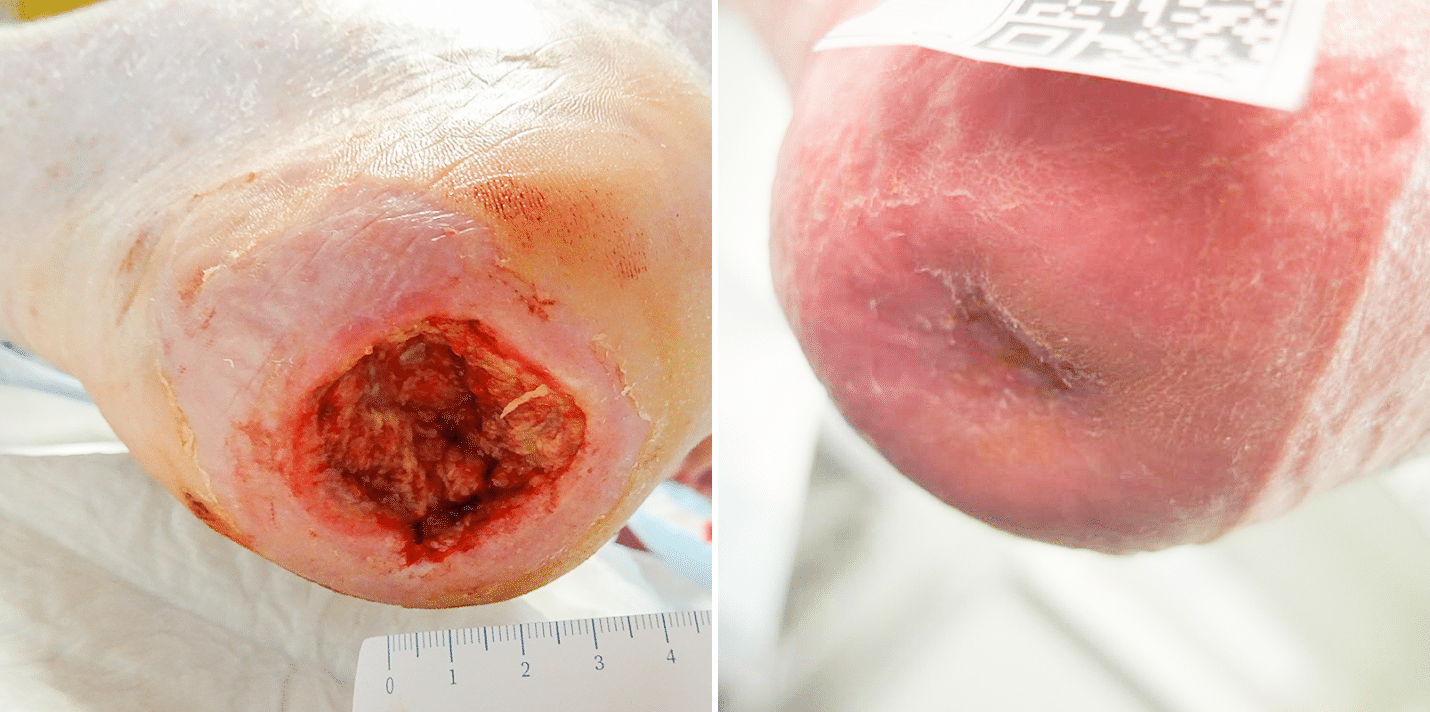
Heel ulcer probe to bone
65-year-old-Male, Type 2 Diabetes, Cardiac insufficiency and Hypertension, heel ulcer present for 10 weeks with positive probe to bone test
One 3C Patch® application per week for 9 weeks
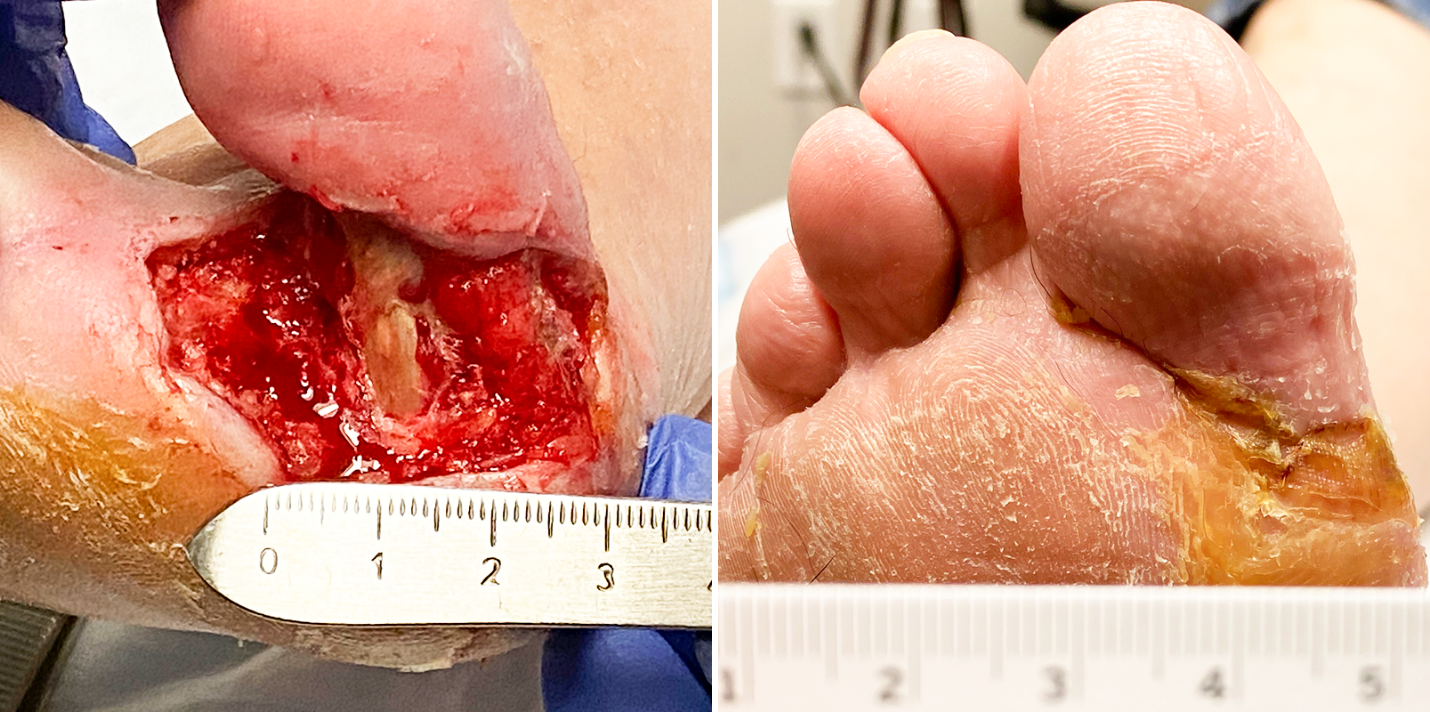
Diabetic foot ulcer – exposed tendon
64-year-old, Female, Type 2 diabetes, diagnosed age 24, Hypothyroid, foot ulcer present for 10 weeks
Five 3C Patch® applications
FAQ
Frequently asked questions
What types of wounds can be treated with 3C Patch®?
Generally, it is possible to treat different types of hard-to-heal wounds (> 4 weeks). Our RCT was designed for treating diabetic foot ulcers with 3C Patch®, and therefore our treatment guidelines and recommendations are related to this type and use.
Can I use a compression bandage combined with 3C Patch®?
Yes, it is possible to use 3C Patch® together with compression therapy. However, as 3C Patch® is an active treatment, it is important to keep an eye on any changes in exudate levels – and change the secondary dressing accordingly.
Can I treat deep ulcers, interdigital ulcers, or ulcers with exposed tendons or bone contact?
Yes, just be sure that the 3C Patch® is placed on a clean well-debrided wound bed, and no osteomyelitis is present. You can also place a part of the patch at the bottom of the wound with the rest of the 3C Patch® up the sides. It is important to stimulate the growth of the ulcer from the bottom.
Can I cut the 3C Patch®into shape so it fits the ulcer?
Yes, no problem: The easiest way is to place the patch on a sterile absorbent layer with the cell side up and cut through this layer and the patch at the same time. This makes cutting and handling the patch very easy.
