Non-healing wounds have an increased chance of healing with 3C Patch®
Non-healing wounds, sometimes referred to as hard-to-heal or difficult to heal wounds/ulcers, fail to progress through the normal healing process and do not close within 4 to 12 weeks.
The Wound Healing Society classifies non-healing wounds into four categories based on their etiology: pressure ulcers, diabetic ulcers, venous ulcers, and arterial insufficiency ulcers.
3C Patch® is a completely proven, 100% autologous wound treatment. The results of the 3C Patch® on hard-to-heal diabetic foot ulcers are supported by a large, international randomized controlled trial.

REDUCES COMPLICATIONS
3C Patch® is a fully autologous cellular-based wound care product
Almost 15% of Medicare beneficiaries (8.2 million) are affected by non-healing wounds, with an annual cost between $28.1 to $31.7 billion. The most expensive estimates seem to be for surgical wounds followed by diabetic foot ulcers. The longer a wound remains unhealed, the greater the risk of complications, reduced QoL for patients, and increased costs.
3C Patch® was created to address this unmet clinical need and reduce the complications associated with non-healing wounds.
The effectiveness and safety of 3C Patch® are backed by robust clinical evidence, including a large, international, multi-center, observer-blind randomized controlled trial. The results of this trial showed that 3C Patch® can significantly improve the chance of healing for non-healing diabetic foot ulcers and reduce the complications associated, including amputations.

HIGHLY EFFECTIVE, PERSONALIZED TREATMENT
3C Patch® is a 100% autologous patch with living cells, proven to significantly increase the chance of healing for non-healing diabetic foot ulcers
The 3C Patch® is created by a fully integrated system – the 3C Patch® System – that draws on the body’s capacity to aid its own healing process and, as such, provides a highly effective, personalized treatment.
With just a small sample of the patient’s blood (18ml), the 3C Patch® System reformulates the blood into a triple-layer patch comprising fibrin, active cells, and growth factors, which are released into the wound.
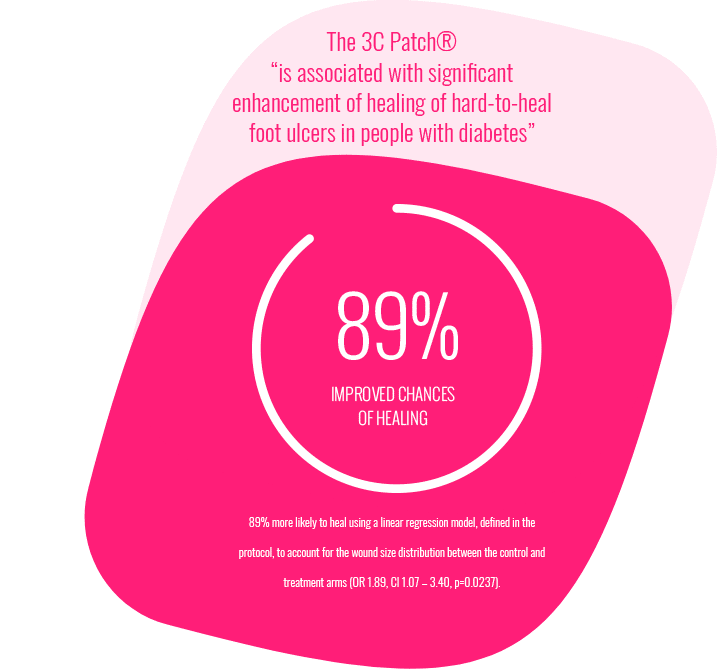
PROVEN TO SIGNIFICANTLY INCREASE THE CHANCES OF HEALING
The 3C Patch® can help stimulate the growth of new granulation tissue
In-vitro studies show that 3C Patch® contains living cells that actively respond to the wound environment, are able to engulf bacteria, promote neovascularization, cell growth, and collagen synthesis. 3C Patch® can help stimulate the growth of new granulation tissue after just a few treatments and increase the chance of complete wound closure.
The effectiveness of the 3C Patch® is supported by the results of a large randomized controlled trial (RCT). 269 patients were included in the study after they went through a run-in period of 4 weeks, during which their wounds showed less than 50% area reduction and thereby classified as non-healing diabetic foot ulcers. The RCT results showed that patients treated with 3C Patch had an 89% improved chance of healing compared to the control group.

3C Patch® Mode of Action
Watch the video explaining how 3C Patch® can help difficult to heal wounds
3C Patch® bridges the gap in non-healing wounds
During normal wound healing, inflammation increases blood flow, and immune cells, platelets, and growth factors reach the wound. This inflammatory response activates the wound healing cascade and clears bacteria and debris. The wound enters the proliferation phase, forms new tissue, and ultimately heals.
If the microvascular flow is impaired, the availability of key blood components decreases, and the wound does not progress to the proliferation phase and does not heal. Approximately 60% of patients with diabetic foot ulcers develop wounds that become hard-to-heal. Applied directly to the wound surface,
3C Patch® provides a high concentration of fibrin, leukocytes, and platelets. Fibrin provides moisture retention; leukocytes are known to fight infection, while platelets are known to provide high growth factor levels and can participate in the resolution of inflammation.
3C Patch® treatment process
The 3C Patch® System produces a 3C Patch® through a remarkably simple and automated process at the point of care. It is easy for clinicians to run treatment steps in parallel – thus securing a time-efficient workflow during the consultation.
1. Draw blood
As soon as the patient has been seated in the treatment room or, if possible, already when the patient is sitting in the waiting area, open the 3C Patch® Kit and draw 18ml blood into the 3C Patch® Device.
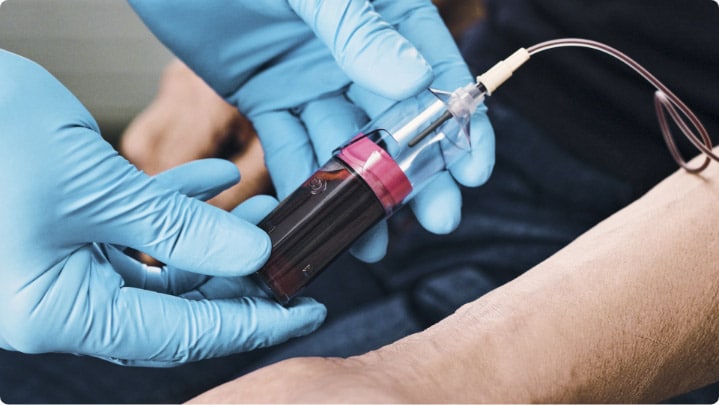
2. Start the 3CP® Centrifuge process
Place the filled 3C Patch® Device in the 3CP® Centrifuge, and press ‘start’ to initiate the automated three-step process: centrifugation, coagulation, compaction.

3. Remove old dressings and perform a thorough debridement
While the centrifuge process is taking place, remove the old dressings, clean the wound and make a thorough debridement using a curette or scalpel to fresh tissue and minor bleeding. The living cells in the 3C Patch® must make contact with fresh tissue in the wound bed so that the signaling substances from the 3C Patch® can have an effect.
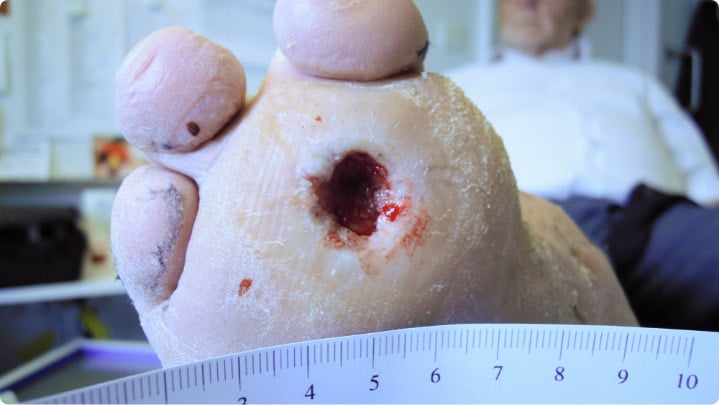
4. Apply 3C Patch® to the wound and cover with dressings
Upon finalization of the centrifugation process, apply the 3C Patch® directly to the wound. Cover it with the supplied non-adherent primary dressing and secure it in place. Apply a secondary absorbent dressing, depending on the exudate level of the wound.
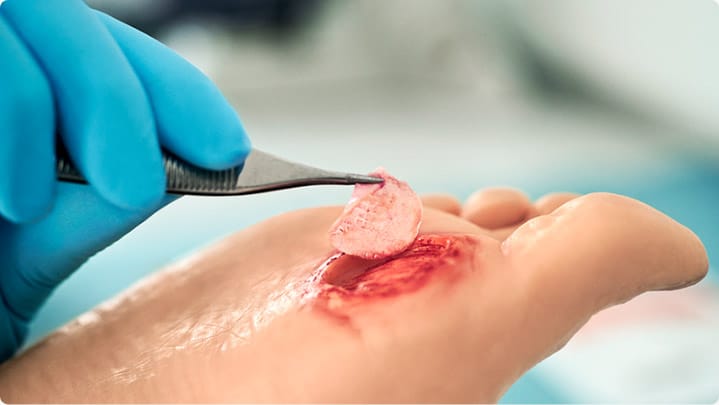
Non-healing wound treatment guidelines
Weekly treatment is recommended according to the results in the 3C Patch® RCT and cohort studies. However, some clinicians are choosing an initial bi-weekly treatment to quickly stimulate the non-healing wound and then switch to weekly treatment when the wound has come out of the chronic phase.
Each 3C Patch® is essentially a delivery vehicle for the cellular components essential to reestablish wound healing. It takes several applications to start having an effect (typically, there is a visible effect after 2-3 treatments).
Our view on the proposed MOA is that whilst 3C Patch® delivers immune cells, platelets, growth factors, and other signaling substances (chemokines and cytokines) to the wound site, these are also known to ‘call-in’ and recruit further cells to the wound, which can potentially lead to granulation tissue forming in the wound, and as shown by the results of the clinical studies, the non-healing wounds close faster than with just standard of care treatment alone.

For optimal results, 3C Patch® should be used in conjunction with standard of care procedures for comprehensive wound management tailored to the specific cause of the wound (such as diabetic, venous, surgical).
Standard of care may include
Removal of necrotic or infected tissue
Off-loading
Compression therapy for venous stasis ulcers
Establishment of adequate blood circulation
Maintenance of a moist wound environment
Management of wound infection
Wound cleansing
Nutritional support, including blood glucose control for subjects with diabetic ulcers
Bowel and bladder care for subjects with pressure ulcers at risk for contamination
Management of underlying disease
3C Patch is FDA cleared and covered by CMS
The 3C Patch® System is intended to be used at point-of-care for the safe and rapid preparation of platelet-rich plasma (PRP) gel from a small sample of a patient’s own peripheral blood.
Under the supervision of a healthcare professional, the PRP gel produced by the 3C Patch® System is topically applied for the management of exuding cutaneous wounds, such as:
leg ulcers,
pressure ulcers,
diabetic ulcers,
mechanically or surgically debrided wounds
FAQ
Frequently asked questions
How do I place a 3C Patch®into the wound?
The “chequered” side of the 3C Patch® facing the filter is the side with the active cells on it, so this is the side that must face downwards in contact with the ulcer.
How long will the growth factors be released in the ulcer?
In Vitro data showed that growth factors are released for up to 7 days.
Can the 3C Patch®be stored or refrigerated?
No, we do not recommend storing the 3C Patch® in a refrigerator or freezer. The 3C Patch® must be stored at room temperature until use and applied within an hour.
How long after drawing the blood should the centrifugation begin?
It is important to start the centrifugation soon after taking the blood in order to separate the cells before coagulation starts. Because our device contains no anti-coagulants or additives, centrifugation should be initiated within approximately 5 min. after the blood draw.
